Sick Role Behavior and Diversity
Sick role behavior is an activity expected of a person who is physically ill, mentally ill, or injured. Such activities are undertaken for the purposes of getting well by those who consider themselves ill and can involve, for example, seeking medical advice, taking time off work and relinquishing responsibility for one’s own care to friends or family.
A concept popularized by Sociologist Talcott Parsons, he noted (in the Social System, 1951) that people in a sick role were expected to cooperate with caregivers and to want to get well, were also provided with an exemption from normal obligations.
He explained that whilst disease involves bodily dysfunction, being sick—that is, being identified and accepted as ill—is a role governed by social expectations, of which he listed four.
- Exemption from normal social role responsibilities that must be legitimated by some authority, often a medical practitioner.
- Exemption from responsibility for being ill, which means that the sick must be looked after.
- Since sickness is deemed undesirable, the sick is obliged to want to get better.
- Seek technically competent help and co-operate in trying to get better.
According to researchers, Parsons’ view of illness and sick behavior as passive fails to address the lay person’s role in the process of their illness, as patient autonomy varies; children, for example are more likely to be passive recipients of medical help than adults. A number of other weaknesses have been exposed in Parsons sick role model, accordingly, the model does not account for differences in gender, sexuality, other cultures, race or class, mental or chronic illnesses, the aged or even pregnancy.
Medical experts studied and investigated cultural diversity in beliefs about sick role behaviors and as predicted, when asked to generate sick role behaviors and rate these in terms of their importance, whites and minorities did not differ in the number or type of causes they generated or in the importance rating they assigned to these. Cultural differences and diversity in causal attributions related to sick role behaviors are examined, and the roles of methodology in determining such behaviors are highlighted.
Africans


Illness is intertwined with cultural and religious beliefs, and healing is holistic in nature. It does not focus only on the physical condition, but also on the psychological, spiritual, and social aspects of individuals, families, and communities.
When patient suffers, he does not suffer alone but with the corporate group. Whatever happens to the individual happens to the whole group, and whatever happens to the whole group happens to the individual. Treatment can be strengthened by spiritual beliefs of sick person who already exhibit these beliefs. Patients are directed to use the belief positively to improve their illness. Also, the belief can be guided by clinicians to help in illness recovery.
African Americans


Illness means that usual roles cannot be fulfilled; based on one’s inability to work. Attention from family and relatives expected, but independence maintained. Family is the center of the Community. Immediate and extended family may attend medical appointments with loved ones. Healthcare decisions may include the wishes of the individual and the family. There is also a very strong sense of shared community.
American Indians


Be sick, quiet, and stoic. Ceremonies play an important role in the overall wellbeing and they involve the patient, the family, and the community in the healing process. Ceremonial gatherings may last for days or weeks; the more people that are present, the greater the healing energy. During times of illness, a medicine man or woman or shaman will be called upon. In most cases the medicine person is also considered a holy person because it is the belief that they do all of their healing with the Creator’s help and guidance. In most cases, both modern medicine and traditional healing ceremonies are performed to achieve wellness.
Arab Americans


Physically sick individuals treated well. Patients expected to assume passive roles in any decisions related to them or others. More preference for spiritual wellbeing over physical wellness, so religious beliefs may also influence a patient’s notions of healing. Patients receive illness with patience, prayers, and meditation. Additional system of folk belief exists and also still prominent in the consciousness of many. Within the traditional view, seen and unseen forces coexist within the material world. Unseen forces, most commonly jinn or evil spirits, are thought to be in operation throughout the material realm, an example will be a widespread belief that bad intentions toward a person can cause illness. Some health disorders are attributed to these unseen forces.
Asian Indians


Illness may be seen as something to be accepted and endured rather than fixes or cured. Consequently patients may be stoic in their expression of pain and while respecting authority of the healthcare provider they fell their own role is passive.
The patient’s sick role cannot be isolated from his/her social settings and familial circumstances. Family helps the patient in coping with the stress and difficulties due to the illness. Family relations and obligations sometimes have a major role in influencing the patient to accept the sick role. Also, family only bears the expenditure of the health care of the patient and is recognized legally as the decision-making authority in opting the suitable health care on behalf of the patient.
Brazilians


Ill person expected to receive attention and care from others. Many illnesses may be attributed to divine intervention or fate. When someone is sick, they are not expected to make decisions about their own health issues. Families handle these decisions. A mainstay of folk medicine is herbal and medicinal teas.
Central Americans


Sick person often assumes passive role, and family members provide care. Disease or illness is as a result of natural scientific phenomena, advocate medical treatments that use sophisticated technology to diagnose and treat disease. Ideally, the patient who is responsible for her/his health would also be given more control and autonomy over its maintenance. If people are convinced that their actions have some effect on their illness, then they are more likely to be involved in decisions and to claim more control over the illness experience
Chinese Americans


Sick role common in the Chinese patient. Family expected to take care of patient, and patient takes a passive role in his/her illness. Emphasis is placed on loyalty to family and devotion to traditions with less emphasis on individual feelings. Illness is seen as a personal burden when a member of the family becomes ill. This indicates that the person taking care of the ailing family member must carry and deal with this added stress. Assessing patient’s kinship relationships and determining which family members are most influential in decision making. When possible, engaging the whole family in discussions that involve decisions and education about care, is very critical.
Cubans
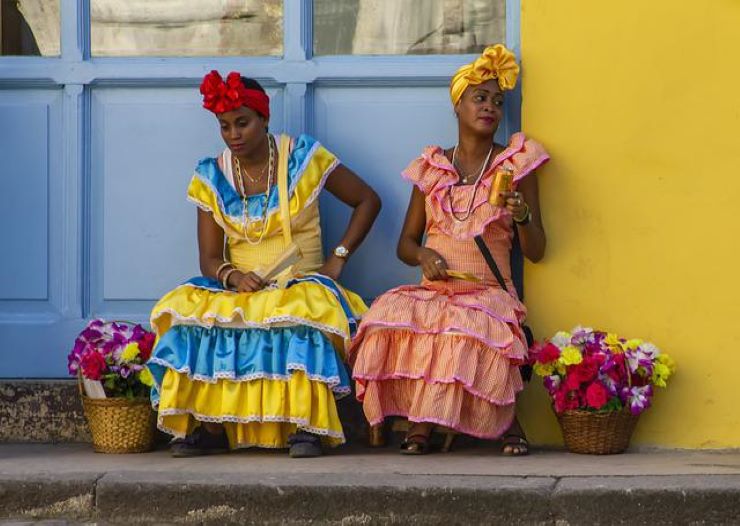
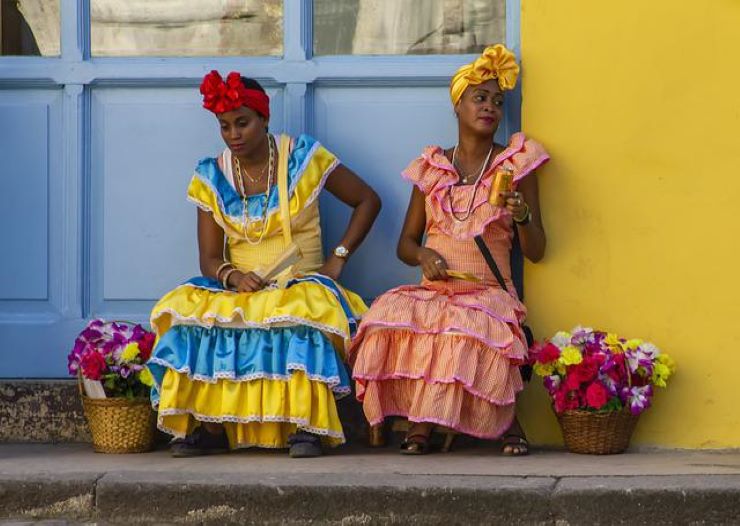
Sick person totally submissive, helpless, and dependent; may even take a passive role in decision making process. Beliefs about illness or disabilities can often be attributed to external causes. Parents or family members may believe that if the patient has a disability, the family members are being punished for their sins. Other family members may accept disabilities as part of a larger divine plan designed by God to make them better persons. Family members who hold these beliefs may be less open to utilizing the services of a health care professional.
Ethiopians


Sick person acts helpless, passive, and totally dependent on family members. Customary to bring home cooked, soothing foods to patient. Family members alter their schedules in order to attend to needs of sick. Health is conceptualized holistically, as an integral phenomenon related to the physiological, psychological, social, and cultural well-being of the individual and the community. Health situations are associated with socio-cultural and religious factors. The individual’s behaviors and interactions with the social, natural, and supernatural powers affect the well-being of the whole group. Each individual is thus responsible not only for him/herself, but also for the well-being and equilibrium of the community.
Filipinos


A sick member of the family is treated well. It is the expectation of the sick to have a family member looking after him/her, to bring food from home that is soothing for the body, for example, rice soup. The patient assumes a passive role where decisions are made for him/her. Older adults tend to cope with illness with the help of family and friends, and by faith in God. Complete cure or even the slightest improvement in an illness is viewed as a miracle. Families greatly influence patients’ decisions about health care. Patients subjugate personal needs and tend to go along with the demands of a more authoritative family figure in order to maintain group harmony.
Haitians
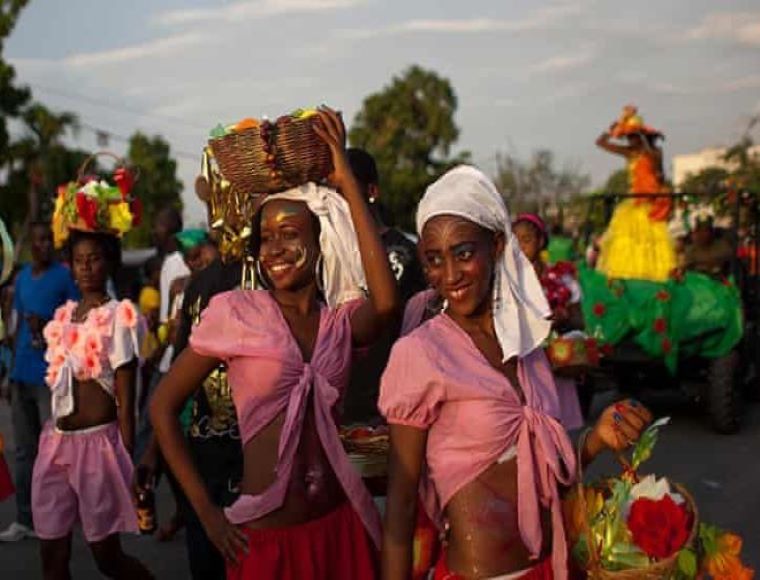
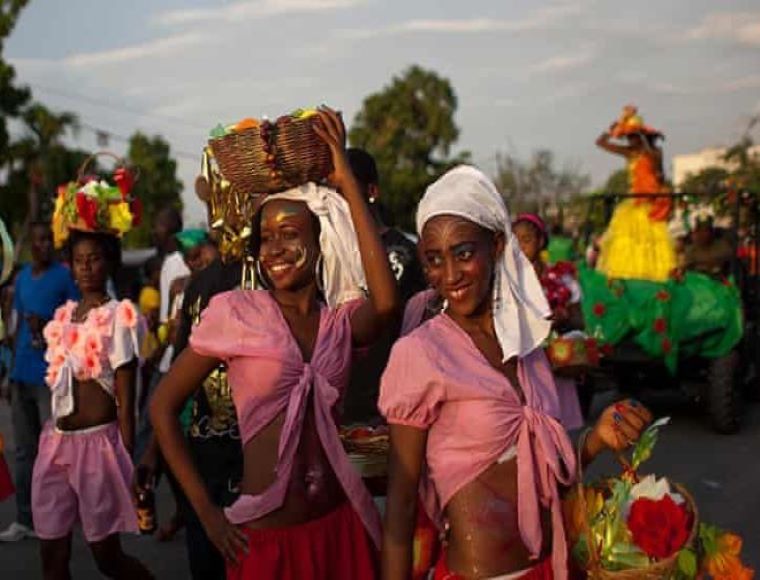
Sick person assumes a passive role and allows others to do for him/her. Family members will rise to the occasion with everyone participating in the care of the loved one. Many believe that God is the ultimate decider of health, illness, life and death. This belief may be manifested as passivity concerning health decisions. Some believe that illness may be caused by either natural or supernatural factors.
Iranians


Patients assume passive role. Bad news generally kept from them. Patient well treated by everyone and looked after. Hope is never taken away. Health seeking behavior is significantly influenced by culture, religion, and socioeconomic status. The important role of family as an influencing factor on illness representations.
Japanese


Sick cared for primarily by women; expectations for performing normal duties lifted. Sick person assumes passive role. Women, however, may continue to do household duties even while sick, although other family members may help. The role of women as caretakers of the sick ‘overrides other roles dictated by the formal kinship structure. Part and parcel of the attitude toward illness is the emphasis on peace and quiet, or bed rest as the major treatment for virtually any illness, from a minor cold to a major disease. People continue to carry out the sick role in their relationship with family members and visitors. Care of the sick is not transferred completely to the hospital. Instead, the people closest to the patients continue to care for them, often day and night, in important ways.
Koreans


Common for family member to behave as very ill, possibly worse than they actually feel, normal for this culture. Again, outsiders may view patient as being dramatic, but this behavior is appropriate in Korean culture. Passivity expected and family takes care of patient’s basic needs. The illness behavior of Korean lay people is characterized by seeking help from multiple sources, noncompliance with medical treatment, preference for magico-religious therapies, use of health foods, and reliance on word-of-mouth advice from lay persons. The author attributes these behaviors to traditional concepts of illness, a viewing that illness and death are a natural part of life. Consult with the family in cases of serious or terminal illness. While the decision making is family focused, the husband, father, eldest son, or daughter may have the final say. The eldest male is often the spokesperson.
Mexicans


Illness seen as social crisis and experience of entire group. Sick roles clearly defined and family care giving accepted. Women may experience more somatic complaints, such as fatigue. Family is very important within this culture. Often times the mother is the one whom decides when to seek medical treatment. Involve the appropriate family members when providing care to the patient. It is an important avenue for expressing love and care. It is usually best to allow family members to spend time with patient and assist the with daily activities. Older family members and other relatives are respected and are often consulted on important matters involving health and illness. Patients may view illness as God’s will or divine punishment brought about by previous or current sinful behavior, preferring the use of home remedies and consulting a folk healer.
Puerto Ricans


Patients usually assume a passive role. Family members must do all care for sick, including preparing caldos (soups, special or favorite foods). Family and close friends take priority and are extremely important. Greatest difficulty in the acceptance of sick role because patients’ spiritual and religious beliefs play a significant part in their approach to health care, illness, and everyday life. Women are viewed as not only culture-bearers but also as primary caregivers and gatekeepers for the health of their families. Many of the population patients seeking medical care first had to talk with or seek assistance from family resources, whether it is for individuals or a community
Russians


Ill family member always taken care of by family; may even bring nutritious and appropriate food from home. In general, ill patients place themselves on bed rest. The patient has a passive attitude towards illness and clearly defined as a sick role. There are strong kinship bonds and everyone in the family provides support and service during a crisis. Decisions are made by the parents or the oldest child. There are no major gender issues; decisions could be made by the mother, father, or eldest son or daughter.
Vietnamese


Patient assumes passive role; cared for by family member. The patient is well taken care of, which includes having everything their own way. Any decision made is based on how it may affect family and relationships. Individuality and autonomy are not included in the decision-making process, even with regard to a particular patient’s own health. The family members, particularly older males, are included in every important decision. Women act as primary providers at the bedside although the entire family may care for the patient. Health is viewed as the result of a harmonious balance between the poles of hot and cold that govern bodily functions. Patients do not readily accept Western health counseling and interventions, particularly when self-disclosure is expected. However, it is possible to accept assistance if trust has been gained.
Source: Culture & Nursing Care: A Pocket Guide 2003.
| Some of the views and opinions expressed here are those of the author and do not necessarily reflect the official policy or position of ifocurs.com. Any content provided by our bloggers or authors are of their opinions and are not intended in any way to malign any race, religion, ethnic group, club, organization, company, individual, anyone or anything. |







